1. Maternal vaccines can protect two people in one shot
Just like when your favorite food is on sale two-for-one at the grocery store, maternal immunization is a deal to get excited about. By getting vaccinated in pregnancy, a mother can simultaneously enhance her own immunity and safeguard her child. Her antibodies, which pass to her baby through the placenta, protect at birth and for months thereafter. In this way, one intervention benefits two people—a rare superpower in public health.
2. They’re a lifeline for young infants when direct vaccination is not an option
When a baby is too young to receive or be fully protected by certain vaccines, maternal immunization can fill the gap. Newborn and young infant immune systems are immature and require time and multiple vaccine doses to mount full defenses against many diseases, which leave the earliest days and months of life un- or under-protected. Fortunately, mom’s mature immune system can do the leg work that baby’s can’t—developing and sharing the lifesaving antibodies that her child needs. (Another fun fact: a mom can share maternal immunization-boosted antibodies with her baby through breast milk too.)
3. They’re saving lives and improving health as we speak
Maternal immunization isn’t new. In fact, it has a long, safe, and successful track record against diseases like tetanus, influenza, and pertussis. Vaccination campaigns and supplementary immunization activities have helped dozens of low- and middle-income countries eliminate maternal and newborn tetanus—an otherwise likely death sentence for mothers and babies. And, COVID-19 has put a spotlight on the importance of including pregnant women in vaccine research and ensuring that expectant mothers, who are more vulnerable to certain diseases, can access safe vaccine protection.
Overall, despite its lifesaving potential, maternal immunization isn’t widely or routinely available in low- and middle-income countries beyond tetanus prevention. So, more work is needed if maternal immunization is to become a more robust part of the maternal and child health toolkit in these settings.
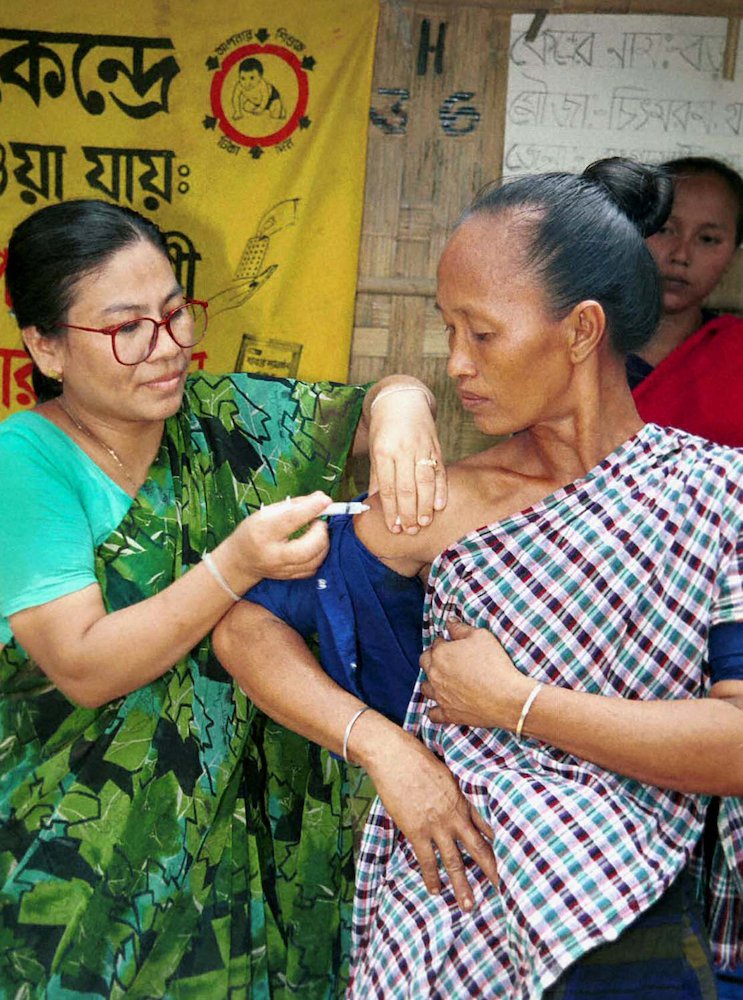
Maternal immunization against tetanus in Bangladesh. Photo: M. Dorgabekova.
4. They’re a way to reach under-served populations
While vaccines save millions of lives every year, traditional immunization programs don’t yet reach all stages of life equitably, including early infancy and pregnancy. Few vaccines can be given at birth or can fully protect in the first days and months of life, and vaccination isn’t even an option for pregnant women in many countries, especially in the poorest parts of the world. Making maternal immunization more commonplace is a promising strategy for covering moms and babies otherwise destined to be missed.
5. They empower moms
Let’s just say it flat out, moms are superheroes. Their strength, courage, wisdom, and love bring us to life and shape the people we become. For all that they are, they deserve to see their children survive and thrive, but also deserve to have access to healthcare tools that help improve the odds. Maternal immunization is one such tool that offers a mother more power and choice to protect her child—and herself while she’s at it.
6. They’re an opportunity to strengthen health services overall
What’s unique about the nature of maternal immunization is that it inherently bridges immunization and antenatal care. The programs that deliver these services, however, operate independently of each other in many low- and middle-income countries and serve different populations—children and mothers. Expanding access to maternal immunization, if done right, could be a chance for these programs to come together in unprecedented ways to harmonize strategies and strengthen overall health care. Benefits could include leveraging resources to improve antenatal care and vaccine services; encouraging pregnant women to attend more well-care visits; and establishing vaccine surveillance systems that also monitor pregnancy and other health outcomes. The trick, however, will be doing so in a way that adds value, not burden, to already under-resourced programs.
“Moms are superheroes. They deserve to see their children survive and thrive, but also deserve to have access to healthcare tools that help improve the odds.”
7. They’re vaccines—so a public health best buy
Preventing disease before it strikes is much more affordable than treating severe illness—and vaccines (including maternal vaccines) are the most cost-effective prevention option around and can contribute to every single Sustainable Development Goal. For every dollar invested in vaccination in the lowest-income countries, an expected US$16 to $18 are saved in healthcare costs, lost wages, and lost productivity due to illness and death. What's more, healthier children do better developmentally and in school—setting them up for brighter futures. Imagine the gains if a platform for routinely delivering maternal vaccines could be established in low- and middle-income countries where infectious diseases take their greatest toll.
8. They’re evolving to meet more needs
Although effective maternal vaccines exist, there’s always room for improvement—and the next exciting maternal vaccine could be right around the corner. New ones are being developed to address pathogens that threaten young children and/or pregnant women—including respiratory syncytial virus (RSV) and Group B Streptococcus (GBS) for which no vaccines are yet on the market. Other efforts are focused on identifying ways that existing maternal vaccines can be used to better meet needs, especially in low- and middle-income countries. Could COVID-19 help normalize vaccine research and use in pregnancy for the foreseeable future? On the edge of your seat? Us too.
9. They prevent illness in stages of life when illness can hit the hardest
By design, maternal vaccines are important for preventing diseases that disproportionately affect infants and pregnant women. A child’s first days and months of life are the most vulnerable with roughly 75% of under-five deaths occurring in year one, mostly in low- and middle-income countries. Among other complications, certain infectious diseases are particularly dangerous in infancy—including tetanus, pertussis, sepsis, meningitis, pneumonia, and severe respiratory disease due to RSV and GBS to name a few. Pregnant women are also at increased risk of severe illness if infected by certain pathogens, including influenza virus and COVID-19. Although not all diseases are preventable through maternal immunization, we’re working across the maternal vaccine development-to-adoption continuum at PATH to address some of the most important diseases that are.
10. They’ve a lot of good yet to do
Unlike interventions at the pinnacle of their potential, maternal immunization is just getting started. Diseases have yet to be tackled—additional evidence yet to be generated—maternal vaccines yet to be licensed—global and country decisions yet to be made—delivery platforms yet to be established—champions yet to be mobilized—women and children yet to be served—and lives yet to be saved. This may seem like a lot to do, but at PATH we prefer to think of it as having a lot to gain. So, what’s next to do? A roadmap from our Advancing Maternal Immunization collaboration has some ideas. Long story short, by coming together now as a global health community across geographies and sectors to overcome remaining hurdles, we can help maternal immunization someday reach its full potential and enable more mothers and infants to live in better health.
Additional resources
- Protecting mothers and infants from infectious diseases fact sheet
- A roadmap for advancing RSV maternal immunization
- Advancing RSV maternal immunization: A gap analysis report
- One shot to stop Group B Streptococcus fact sheet
- Maternal influenza immunization: perceptions of decision-makers, health care providers, and the community in Malawi report
- Maternal influenza immunization: lessons from vaccine introduction and use in El Salvador
- Moving the Needle e-newsletter
- Immunization Matters e-newsletter



